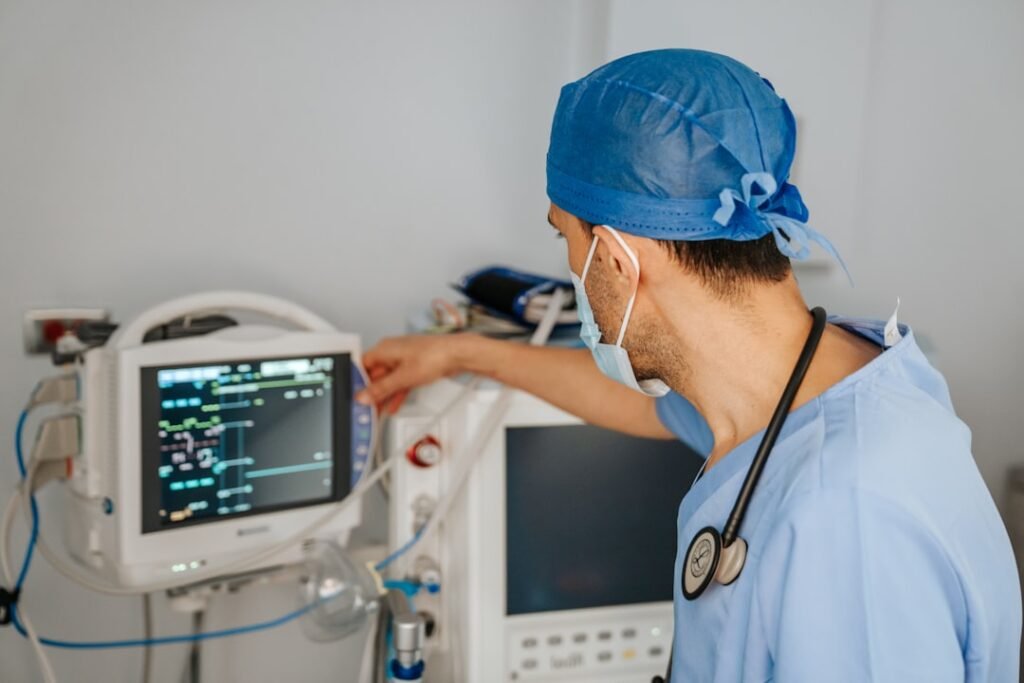
The rapid integration of artificial intelligence across healthcare systems worldwide presents a paradoxical challenge: while AI tools are increasingly prevalent in diagnostics, administration, and patient management, robust evidence confirming their direct positive impact on healthcare AI patient outcomes remains conspicuously scarce. This disjunction between enthusiastic adoption and rigorous validation raises fundamental questions about efficacy, resource allocation, and the ultimate value proposition of these technologies. As hospitals deploy AI for tasks ranging from note-taking to interpreting complex medical imagery, a critical gap emerges in our understanding of whether these advancements genuinely translate into improved patient well-being, reduced mortality, or enhanced quality of life, rather than merely boosting operational efficiency.
75%
Estimated AI tools lacking robust clinical evidence for direct patient benefit
150+
AI-driven medical devices approved by the FDA, highlighting rapid regulatory acceptance
3-5 Years
Typical duration required for comprehensive clinical trials to prove AI efficacy in human health
The Promise vs. The Proof: Navigating Healthcare AI’s Efficacy Gap
The allure of AI in healthcare is undeniable. From automating administrative tasks like note-taking to powering advanced diagnostic tools that interpret X-rays and MRI scans, the technology promises a revolution in efficiency and precision. Proponents highlight AI’s capacity to process vast datasets, identify subtle patterns, and flag potential issues far quicker than human counterparts. Yet, this enthusiasm often overshadows a critical question: how do these technical improvements translate into tangible benefits for patients? The challenge lies not in AI’s ability to perform specific functions, but in rigorously demonstrating that these functions lead to better health outcomes, fewer medical errors, or enhanced patient experiences. The rapid market penetration of these tools, reminiscent of the swift global expansion seen in sectors like electric vehicles, where a company’s BYD electric vehicle growth strategy quickly reshaped the automotive landscape, often outpaces the methodical, often years-long process of clinical validation required to ascertain true efficacy and safety in human health.
Unpacking the Validation Challenge for Healthcare AI Patient Outcomes
Establishing the direct impact of healthcare AI patient outcomes is inherently complex. Unlike a new drug, which undergoes stringent randomized controlled trials (RCTs) to prove efficacy against a placebo or existing treatment, AI tools are often integrated incrementally into existing workflows. Isolating the AI’s specific contribution to a patient’s recovery or improved health from myriad other clinical factors becomes a formidable methodological hurdle. Factors such as the treating physician’s expertise, patient adherence to treatment, and the overall hospital environment all confound attempts to attribute outcomes solely to AI intervention. Furthermore, the dynamic nature of AI models, which can learn and adapt over time, complicates static validation. A model proven effective on one dataset might perform differently on another, especially when encountering new patient demographics or evolving disease patterns. This necessitates continuous monitoring and re-validation, a process that is both resource-intensive and often overlooked in the rush to deploy new technologies.
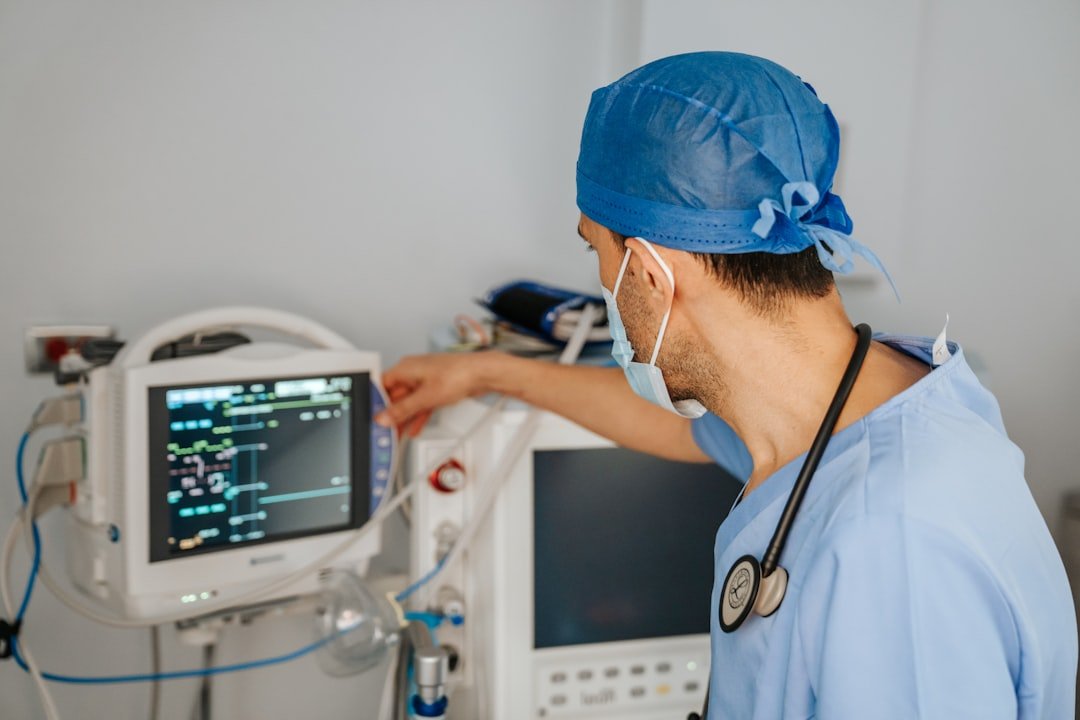
Regulatory Lags and Ethical Imperatives in AI Deployment
The regulatory landscape for healthcare AI is still evolving, struggling to keep pace with the rapid technological advancements. While bodies like the FDA have approved numerous AI-driven medical devices, their focus has primarily been on safety and technical performance, rather than the long-term, real-world impact on patient outcomes. This creates a vacuum where innovative tools can enter the market without the comprehensive efficacy data that would be demanded of other medical interventions. Beyond regulatory frameworks, the ethical implications of unvalidated AI are profound. Issues of algorithmic bias, data privacy, and accountability become paramount when AI systems directly influence patient diagnoses and treatment plans. For instance, an AI trained on predominantly Western datasets might perform poorly when applied to patient populations with different genetic predispositions or lifestyle factors, potentially exacerbating health disparities. Understanding the nuances of cultural differences in AI adoption and performance is crucial here, as a ‘one-size-fits-all’ approach can have detrimental consequences when patient lives are at stake. Ensuring transparency in AI’s decision-making process and establishing clear lines of responsibility when errors occur are ethical imperatives that demand immediate attention.
Beyond the Hype: Defining and Measuring True Patient Value
For healthcare AI to truly deliver on its promise, the industry must shift its focus from mere technical prowess and efficiency gains to a more rigorous definition and measurement of true patient value. This entails moving beyond metrics like diagnostic speed or accuracy rates to quantifiable improvements in health status, quality of life, and reductions in morbidity and mortality. For example, an AI tool that identifies early signs of disease is only truly valuable if that early detection leads to more effective treatment, better survival rates, or a significant improvement in the patient’s long-term health trajectory. Similarly, AI-powered administrative tools must demonstrate not just time savings for clinicians, but also how that reclaimed time translates into more personalized patient care or reduced clinician burnout, indirectly benefiting patients. This requires a patient-centric design philosophy from the outset, where the ultimate goal of improved human health guides every stage of AI development, deployment, and evaluation. Without this clear articulation of value and the metrics to measure it, AI risks becoming an expensive, unproven addition rather than a transformative force in healthcare.
Charting a Course for Responsible Healthcare AI Integration
To bridge the current efficacy gap and ensure that healthcare AI genuinely serves patient interests, a multi-faceted approach is essential. Firstly, there is an urgent need for standardized validation frameworks that mandate rigorous clinical trials, akin to those for pharmaceuticals, tailored to the unique characteristics of AI. These frameworks must account for the adaptive nature of AI and include provisions for continuous monitoring and re-validation in real-world settings. Secondly, greater collaboration between AI developers, clinicians, regulatory bodies, and patient advocacy groups is crucial to define relevant outcome measures and design studies that reflect diverse patient populations. Thirdly, transparency in AI algorithms, data sources, and performance metrics must become a non-negotiable standard, fostering trust and enabling critical evaluation. Finally, investment in robust health data infrastructure and interoperability is foundational, ensuring that high-quality, diverse data is available for training, testing, and continuously improving AI models. By prioritizing demonstrable patient benefit over rapid deployment, the healthcare sector can ensure that AI becomes a truly transformative and trustworthy ally in improving global health.
| AI Application Area | Current Adoption Level | Evidence for Direct Patient Benefit |
|---|---|---|
| Radiology Image Interpretation | High (for anomaly detection & speed) | Emerging, mostly indirect (e.g., faster diagnosis) but limited for long-term clinical outcomes |
| Clinical Note-Taking & Documentation | Growing (for efficiency & burnout reduction) | Indirect/unproven (e.g., impact on care quality via clinician time savings needs validation) |
| Predictive Analytics (Risk Scoring) | Moderate (for population health management) | Variable, context-dependent; robust evidence for individual patient outcome improvement often lacking |
| Drug Discovery & Research | High (in early-stage compound identification) | Long-term, prospective; clinical success still requires traditional trial phases post-AI discovery |
“The speed of AI adoption in healthcare currently outpaces our rigorous understanding of its direct, measurable impact on patient well-being. We risk integrating powerful tools without fully validating their ultimate clinical value, potentially misallocating resources and eroding public trust.”
— Dr. Anya Sharma, Lead Health AI Ethicist, Global Health Institute
🔬
Clinical Validation Gap
The disparity between rapid AI deployment and the slow pace of robust clinical trials proving patient efficacy.
⚖️
Ethical AI Frameworks
Addressing bias, fairness, transparency, and data privacy in AI systems that directly affect human health outcomes.
📈
Defining Patient Outcomes
Moving beyond efficiency gains to measurable improvements in health, quality of life, and mortality rates.
🏛️
Evolving Regulatory Landscape
The challenge for regulatory bodies to keep pace with AI innovation while ensuring patient safety and efficacy.
← Scroll to explore →
🚀 How A Square Solutions Can Help
Turn Intelligence Into Business Advantage
We build AI-powered digital growth systems that help businesses in India and globally translate emerging intelligence into revenue — through SEO automation, content systems, web infrastructure, and data analytics.
📢 Also accepting business advertising partnerships — if you want your brand in front of our growing audience of tech decision-makers, get in touch.
Frequently Asked Questions
Why is it difficult to prove healthcare AI’s direct patient benefit?
Proving direct patient benefit from healthcare AI is challenging due to the complexity of human health, the multitude of confounding clinical factors, the dynamic nature of AI models, and the ethical difficulties in designing traditional randomized controlled trials for AI interventions. It’s hard to isolate AI’s specific impact from other aspects of patient care.
What are the risks of deploying healthcare AI without robust validation?
Deploying unvalidated healthcare AI carries risks such as misallocation of resources, potential for algorithmic bias leading to health disparities, erosion of patient and clinician trust, and the possibility of integrating tools that do not genuinely improve patient outcomes, or in rare cases, could even lead to unintended harm.
How can regulatory bodies ensure AI efficacy in healthcare?
Regulatory bodies can enhance AI efficacy assurance by developing standardized, AI-specific clinical validation frameworks that go beyond technical performance, mandating continuous post-market surveillance, requiring transparency in AI model development and data usage, and fostering international collaboration for consistent standards.
What role do data and transparency play in validating healthcare AI patient outcomes?
High-quality, diverse, and representative data are fundamental for training and validating AI models to ensure their generalizability and fairness. Transparency in how AI models are built, the data they use, and their decision-making processes is crucial for clinicians and regulators to understand, trust, and ultimately validate their real-world impact on patient outcomes.